Contraception options are her choice, but not at the expense of being ill informed.
Two Tauranga women have expressed their concerns over the lack of information they've been given about their options of contraception.
Cayla Euinton, 25, says she originally asked to be put on a combined oral contraceptive pill several years ago, as a way to control her menstrual cycle while travelling overseas.
'Before I was on any form of contraceptive, when on my period I would have a shower and be fine,” she says. 'Then I'd get out of the shower and have to lay on the floor for an hour, because it was that painful.
'When I was travelling I really didn't want to have to deal with that.”
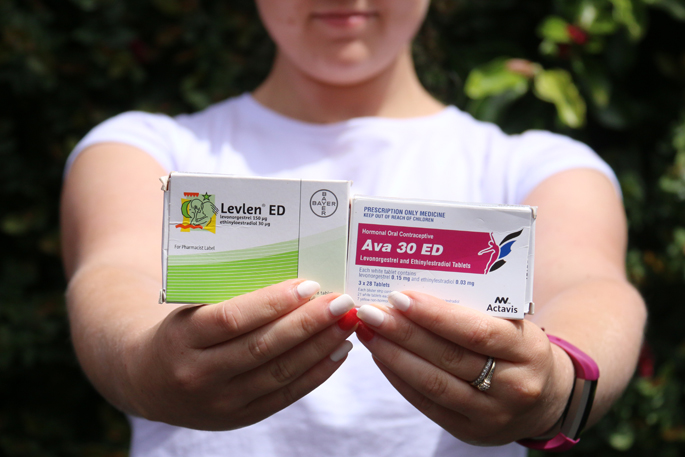
She says her doctor put her on Ava 20, which worked well while she was on her travels, but when she got back she started having issues with spotting.
'When I went back, the doctor was frustrating and just put me on Ava30 and told me to wait it out, which wasn't helpful. So I just stopped taking it, because at the time I wasn't sexually active, so it didn't matter.”
She later went back on Ava 30, prescribed by a different doctor, but wasn't given any information about her prescription or about other options of contraceptives. She says it was just assumed that she had all the information, because she'd already taken it previously.
'I went to a religious school,' she explains, 'so contraceptives were never talked about. I thought there was only one type of pill.
'For example, nobody told me you can't have grapefruit while you're on it, or whether you have to make sure you take it around the same time every day. No-one explained what would happen if you skip one.”
Family Planning national medical advisor Rose Stewart says the issue with GPs is that local practices don't necessarily have someone who specialises in women's health.
'I don't want to cast any assumptions on general practice, because they're really great, but they can be really busy and have shorter appointments,” says Rose. 'Practitioners only have two minutes to give you the information you need.”
She says in some cases, too much information can be confusing, which is often why practitioners resort to more written information, such as pamphlets and websites.
'When people come in, sometimes they can take in a lot of information, but other times they can't or don't want to for all sorts of reasons.”
Rose says everyone is different, so it is a nurse's job to assess what will work best for the patient.
'We judge how much information to give them by their responses,” she says. 'If people ask lots of questions, then you know that they are understanding and they want more information, but if they're not asking a lot of questions, you give them the minimum amount of information and give them written information that is simple.”
Sam Gardner, 25, has also had similar issues to Cayla. She was started on the pill, but later changed to the Depo Provera injection after she found the pill wasn't working for her.
'I used to get three periods a month,” she says, 'and I thought the pill wasn't right for my body. But it turns out I had never been told how to take it properly.
'One of my friends recommended the Depo injection. All I knew about it was that it stopped your period and was a pretty strong form of contraceptive.”
To begin with, the injection was effective, but over time she started suffering from constant pains.
'I was on it for four years, and then went off it because it was making me really sick,” she says. 'I was getting really bad pains without any period.”
While continuing that form of contraception, she also heard that if you're on the injection for too long it can cause infertility.
Rose says Depo injects progestogen into your body, which is similar to one of the hormones produced naturally by a woman's ovaries. It prevents pregnancy by stopping the ovaries releasing an egg each month, as well as changing the lining of the womb.
'This also means your natural fertility can take some time to return to normal after stopping the injections,” says Rose. 'On average, this will be six months but can take up to two years.”
The choice of contraceptive is completely up to the woman, however in some cases the woman will not be advised to choose another option if it will affect her health.
'Sometimes there are medical reasons why people can't use something, and that relates more to the pill than anything else.
'For example, if someone has certain types of migraines, it's really unwise to be on the pill because it could cause a stroke.”
Rose says it's important for practitioners to take a medical history and to inform people of the different methods and potential side effects, if any.
'If you're taking any medicine you're entitled to have full information about it, and the good thing now is that information is available online for everyone.
'Contraceptive is very objective. We can't say what will happen, but we can say if you're feeling different and you're not really happy with it, you need to come back and tell us about it.”


0 comments
Leave a Comment
You must be logged in to make a comment.